The BCG vaccine is the only TB vaccine currently available, although there are other TB vaccines under development. Although far from perfect, the BCG vaccine is a relatively inexpensive, safe, and readily available vaccine that is still the only vaccine available for the prevention of human forms of TB.
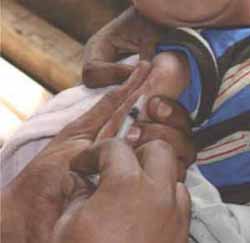
A child being given the BCG vaccine in their upper right arm © AMREF Demsissew Bizuwork
The BCG vaccine is normally given to children as it has been shown to provide very good protection against the disseminated forms of TB in children, including TB meningitis. However the protection provided against pulmonary TB in adults is very variable. So the vaccine is not generally given to adults.1“Immunization surveillance, assessment and monitoring”, WHO www.who.int/immunization_monitoring/diseases/tuberculosis/
The BCG vaccine is one of the most widely used of all current vaccines, and overall it reaches more than 80% of all new born children and infants in countries where it is part of the national childhood immunization programme.2“BCG vaccine”, WHO www.who.int/biologicals/areas/vaccines/ The World Health Organisation (WHO) monitors the estimated coverage of the BCG vaccine in every country. 3“Estimates of BCG coverage”, WHO //apps.who.int/immunization_monitoring/globalsummary/timeseries/tswucoveragebcg.html
Not every country that could do so gives the vaccine to all children. Generally countries where there is a high level of TB use the BCG vaccine to vaccinate all children. Some countries with a low level of TB, such as the United States and England do not give all children the vaccine, but only those considered at particular risk. The United States has never vaccinated all children, but in the United Kingdom all children were given the vaccine until 2005.4“The BCG World Atlas”, www.bcgatlas.org/index.php
A bottle containing BCG vaccine
People who have had the vaccine will often then have a positive result to a TB skin test. This makes it more difficult to establish whether someone has latent TB. This is one of the reasons that the vaccine is not used in some countries.5“When is the BCG (TB) vaccine needed? - Vaccinations - NHS Choices”, NHS choices www.cdc.gov/tb/topic/testing/
The skin test will often be given before BCG vaccination. If there is a positive result to the skin test indicating that the person already has some immunity to TB, then the BCG vaccination will not be given. Giving the vaccine to someone who already has some immunity, provides no benefit and could cause unpleasant side effects.6“BCG (tuberculosis) vaccination - When it is needed”, NHS Choices, www.nhs.uk/Conditions/BCG/Pages/When-it-is-needed.aspx
There has been a shortage of the BCG vaccine in the European Union since April of 2015. It is now not expected that supplies will return to normal until 2017.7“100,000 babies lose out due to lack of TB jab”, Independent.ie, www.independent.ie/irish-news/health/ In England it is said that supplies of BCG ran out in the summer of 2016.
In the early years of the use of the vaccine there were some concerns about safety, and there was the Lubeck disaster. Subsequently for many years there was little concern about safety. However it is now considered that the use of the BCG vaccine in children who are immune compromised, such as children with HIV, could result in them having an infection caused by the BCG vaccine itself. This is because the BCG vaccine contains a live but very weakened form of a bacteria called Mycobacterium bovis. This is not the same bacteria though as the bacteria that causes TB in humans, which is called Mycobacterium tuberculosis.8BCG - the current vaccine for tuberculosis, WHO www.who.int/vaccine_research/diseases/tb/vaccine_development 9“The Difference Between Latent TB Infection and Active TB Disease”, CDC, www.cdc.gov/TB/publications/factsheets/general/LTBIandActiveTB.htm
BCG immunization generally causes some pain and scarring at the site of the injection.
The organisation AERAS was set up in 2003 to develop new, safe, effective and affordable vaccines to replace the BCG vaccine. A new vaccine will need to protect against all strains of TB including the different types of drug resistant TB. The vaccine will also need to be suitable for use in preventing TB in children, adolescents and adults, as well being safe for use in people who are infected with both HIV and TB.10“AERAS - Global Efforts”, AERAS www.aeras.org/about-tb/global-efforts.php
AERAS is supporting the clinical testing of six possible new TB vaccines any one of which could be a suitable vaccine to replace BCG. In October 2012 it was announced that in connection with Glaxo, AERAS will in 2013 begin a phase IIB study in Kenya, India and South Africa. It is planned that this vaccine if successful would be used alongside the existing BCG vaccine.11“Aera, GSK will test TB vaccine in India and Africa”, Vaccine News Daily, October 12 2012 vaccinenewsdaily.com
Another potential TB vaccine also designed to be used in conjunction with BCG is MVA85A. In February 2013 the results were announced of a phase 2B trial of MVA85A.12“Safety and efficacy of MVA85A, a new tuberculosis vaccine, in infants previously vaccinated with BCG: a randomised, placebos-controlled phase 2B trials”, The Lancet, February 4 2013 www.thelancet.com/ This disappointingly showed that MVA85A did not provide any significant effectiveness against either tuberculosis or M. tuberculosis infection, although some people considered that:
“the findings … are not a terminal prognosis for MVA85A, or for any of the other tuberculosis vaccines in development.”13“A major event for new tuberculosis vaccines”, The Lancet, February 4 2013 www.thelancet.com/
Would you like to send us a comment about this page?
| 1. | ↑ | “Immunization surveillance, assessment and monitoring”, WHO www.who.int/immunization_monitoring/diseases/tuberculosis/ |
| 2. | ↑ | “BCG vaccine”, WHO www.who.int/biologicals/areas/vaccines/ |
| 3. | ↑ | “Estimates of BCG coverage”, WHO //apps.who.int/immunization_monitoring/globalsummary/timeseries/tswucoveragebcg.html |
| 4. | ↑ | “The BCG World Atlas”, www.bcgatlas.org/index.php |
| 5. | ↑ | “When is the BCG (TB) vaccine needed? - Vaccinations - NHS Choices”, NHS choices www.cdc.gov/tb/topic/testing/ |
| 6. | ↑ | “BCG (tuberculosis) vaccination - When it is needed”, NHS Choices, www.nhs.uk/Conditions/BCG/Pages/When-it-is-needed.aspx |
| 7. | ↑ | “100,000 babies lose out due to lack of TB jab”, Independent.ie, www.independent.ie/irish-news/health/ |
| 8. | ↑ | BCG - the current vaccine for tuberculosis, WHO www.who.int/vaccine_research/diseases/tb/vaccine_development |
| 9. | ↑ | “The Difference Between Latent TB Infection and Active TB Disease”, CDC, www.cdc.gov/TB/publications/factsheets/general/LTBIandActiveTB.htm |
| 10. | ↑ | “AERAS - Global Efforts”, AERAS www.aeras.org/about-tb/global-efforts.php |
| 11. | ↑ | “Aera, GSK will test TB vaccine in India and Africa”, Vaccine News Daily, October 12 2012 vaccinenewsdaily.com |
| 12. | ↑ | “Safety and efficacy of MVA85A, a new tuberculosis vaccine, in infants previously vaccinated with BCG: a randomised, placebos-controlled phase 2B trials”, The Lancet, February 4 2013 www.thelancet.com/ |
| 13. | ↑ | “A major event for new tuberculosis vaccines”, The Lancet, February 4 2013 www.thelancet.com/ |